By Andrew Parkin, Environics Institute and Justin Savoie, University of Toronto.
The COVID-19 pandemic had both immediate and lingering impacts on our health. The immediate ones were all too obvious: millions died or became seriously ill. While some recovered quickly, others experienced persistent symptoms for months, if not years. Combined with these physical effects was the toll the pandemic took on people’s mental health, as they faced loss and grief, exposure to new health risks, restrictions on regular activities, social isolation, economic strains and prolonged uncertainty.
The pandemic, as an official emergency, is technically over, though the virus continues to circulate. The various public health restrictions imposed in the first years of the pandemic have long since been lifted. Workplaces and schools have fully re-opened, travel for business and tourism has resumed, and sports and entertainment venues are eager to welcome as many spectators as they can. While some are still feeling the physical health impacts of COVID-19, most people have resumed their pre-pandemic lifestyles. Given this, is it reasonable to expect that the wider mental health effects have now faded as well?
The results of several health-related questions from a recent Canadian survey suggests not. In fact, it appears that, despite the passage of time since the height of the pandemic, past experiences with COVID-19 may today be more likely to be associated with poor mental health than with poor physical health.
The survey, conducted early in 2024, asked 2,200 adult Canadians whether they had ever been sick with COVID-19 – and, if so, whether their illness was serious. Just over one in two (54%) said they had had COVID. (This is fewer than the actual proportion, as many are not aware that they were infected, especially if this occurred after vaccination.) Of these, 30 percent say their case was serious.
The total adult population thus divides as follows:
- 46% say they had not had COVID-19 (or say they don’t know);
- 38% say they had COVID-19, but it was not serious; and
- 16% say they had COVID-19 and it was serious.
It appears that, despite the passage of time since the height of the pandemic, past experiences with COVID-19 may today be more likely to be associated with poor mental health than with poor physical health.
The results of several health-related questions from a recent Canadian survey suggests not. In fact, it appears that, despite the passage of time since the height of the pandemic, past experiences with COVID-19 may today be more likely to be associated with poor mental health than with poor physical health.
The survey, conducted early in 2024, asked 2,200 adult Canadians whether they had ever been sick with COVID-19 – and, if so, whether their illness was serious. Just over one in two (54%) said they had had COVID. (This is fewer than the actual proportion, as many are not aware that they were infected, especially if this occurred after vaccination.) Of these, 30 percent say their case was serious.
The total adult population thus divides as follows:
- 46% say they had not had COVID-19 (or say they don’t know);
- 38% say they had COVID-19, but it was not serious; and
- 16% say they had COVID-19 and it was serious.
Experiences with COVID-19
The proportion that reports having had a serious case of COVID-19 is slightly higher for women (18%) than for men (14%), for those under the age of 45 (21%) than for those age 45 and older (12%), and for those with children living with them (21%) compared to those without children at home (14%).
The survey has no way of medically assessing the health of participants; it simply asks people about the state of their physical and mental health, and other aspects of their well-being.
Overall, 39 percent of adult Canadians report that their physical health is either excellent or very good. Almost as many (36%) describe their physical health as good, and about one in four (24%) say it is only fair or poor. The proportion that describes their physical health as fair or poor, however, is somewhat higher for those who had a serious case of COVID-19 at some point since the start of the pandemic in March 2020 (30%), compared to those who had a non-serious case (24%) or who do not report having had COVID-19 at all (22%).
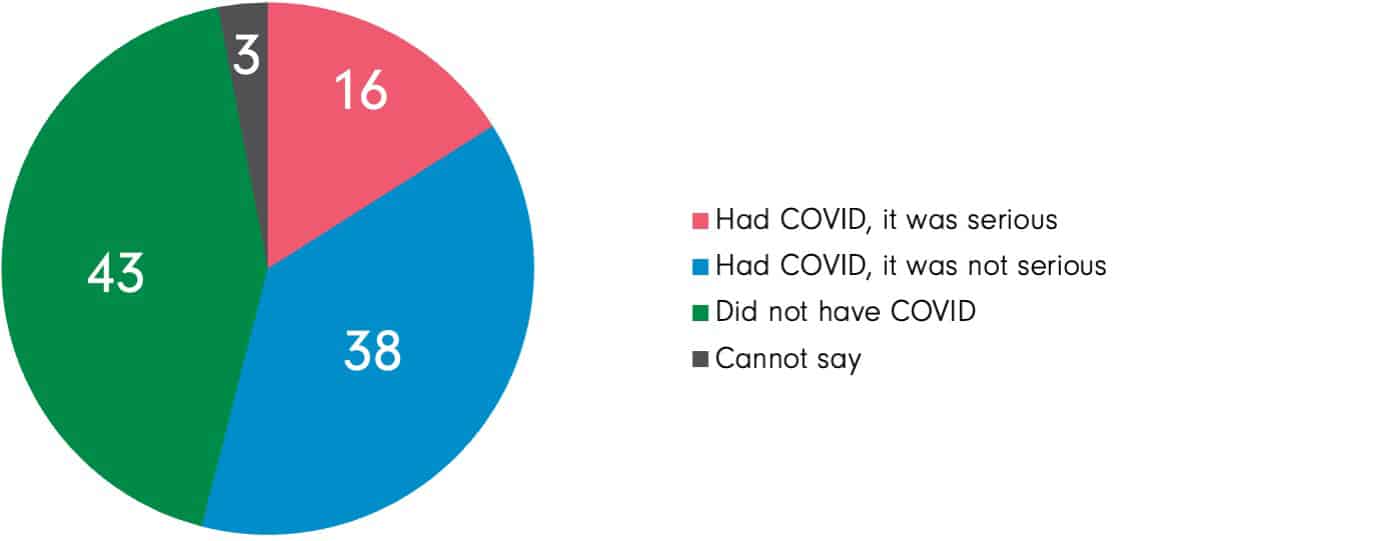
C6. Since the start of the pandemic in Canada in March 2020, have you ever been sick with COVID-19?
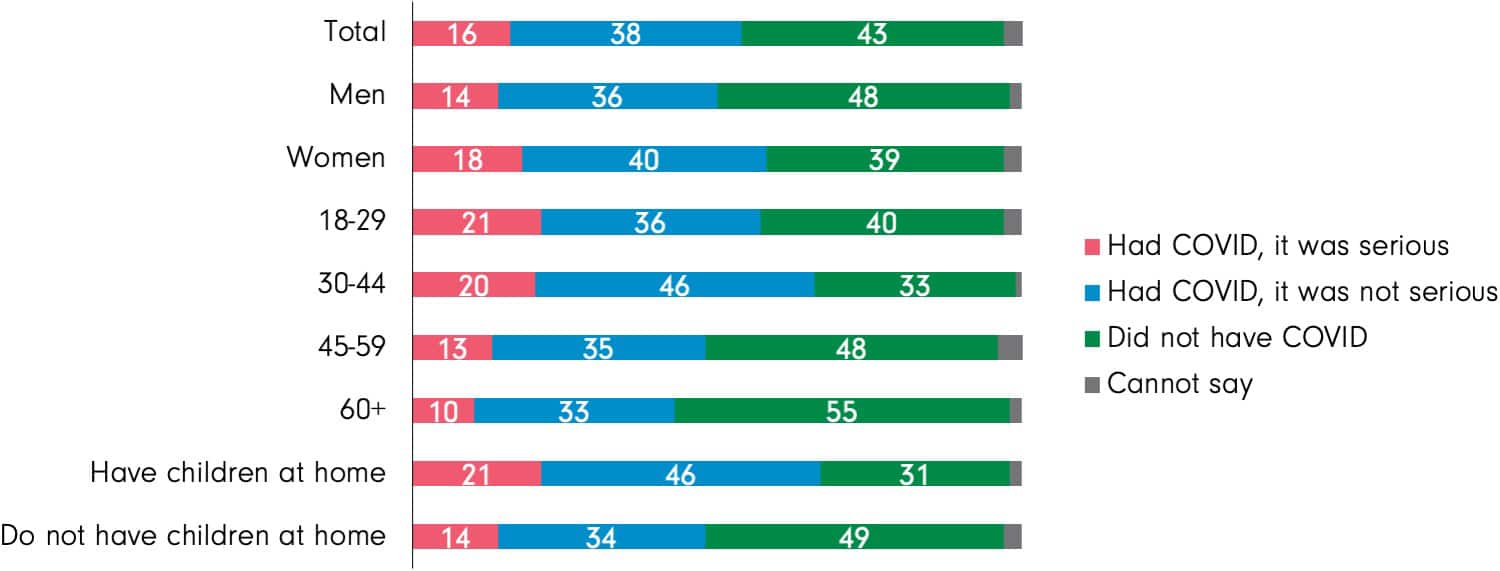
C7. How serious was your illness due to COVID-19?
This finding is not that surprising: there seems to be a relationship between having been seriously ill with COVID-19 after March 2020, and the likelihood of reporting poor physical health today. This relationship could exist either because COVID-19 has lasting physical health impacts for some, or because people with pre-existing health conditions were more likely to be seriously impacted by the COVID-19 virus. (It could also be that people with poor health are generally more sensitized to health risks, and therefore are more likely to assess their experience with COVID-19 as serious.)
What is perhaps more surprising is that the same relationship exists today in the case of mental health. More than two in five adult Canadians (44%) report that their mental health is excellent or very good. But this proportion is significantly lower for those who had a serious case of COVID-19 (36%) or who had a non-serious case (38%), compared to those who do not report having had COVID-19 at all (53%). Conversely, one in four adult Canadians (25%) report that their mental health is fair or poor. But this proportion is significantly higher for those who had a serious case of COVID-19 (35%), compared to those who had a non-serious case (28%) or who do not report having had COVID-19 at all (20%).
What’s more, the difference between those reporting having had a serious case of COVID-19 and those who do not report having had it at all is greater when it comes to the incidence of poor mental health (a difference of 15 percentage points in the proportion reporting fair or poor mental health) than to the incidence of poor physical health (a difference of 8 points).
COVID and physical and mental health
The same pattern holds when it comes to three other measures of well-being. The survey asked how frequently people might feel anxious, depressed or lonely. In each case, those who report having had a serious case of COVID-19 are much more likely to also report having had these feelings at least three days in the past week.
Specially, compared to those who do not report having had COVID-19 at all, those who say they had been seriously ill with COVID-19 are:
- 20 percentage points more likely to say they felt anxious at least three days in the past week (43%, compared to 23%);
- 15 percentage points more likely to say they felt depressed at least three days in the past week (32%, compared to 17%); and
- 11 percentage points more likely to say they felt lonely at least three days in the past week (30%, compared to 19%).
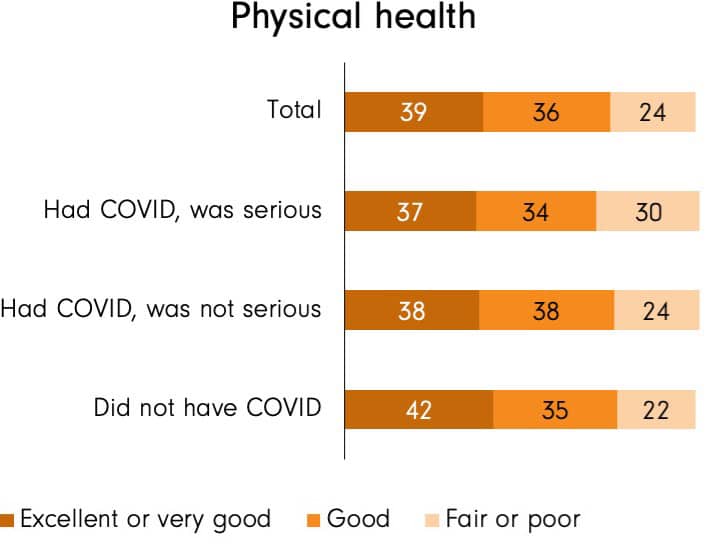
C3. In general, would you say your physical health is excellent, very good, good, fair, or poor?
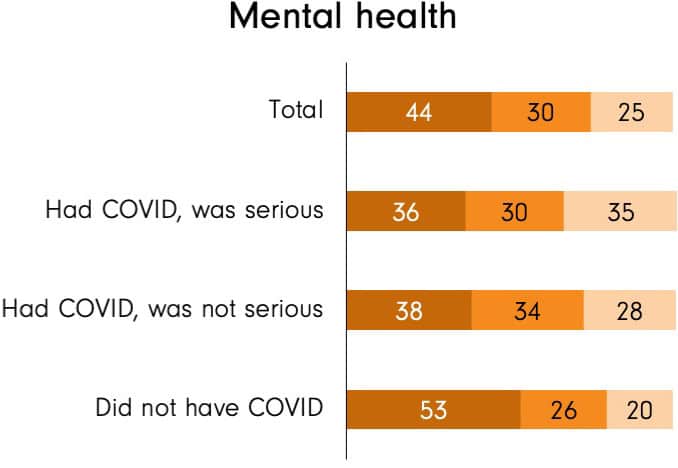
C4. In general, would you say your mental health is excellent, very good, good, fair, or poor?
COVID and well-being
As noted, women and younger Canadians are more likely to report having had a serious case of COVID-19. But they are also more likely to report poor mental health. A more detailed analysis confirms, however, that this does not account for the relationship between having had a serious case of COVID-19 and poorer (self-reported) mental health. This relationship remains significant even when we control for demographic factors such as age and gender, as well as region and education.
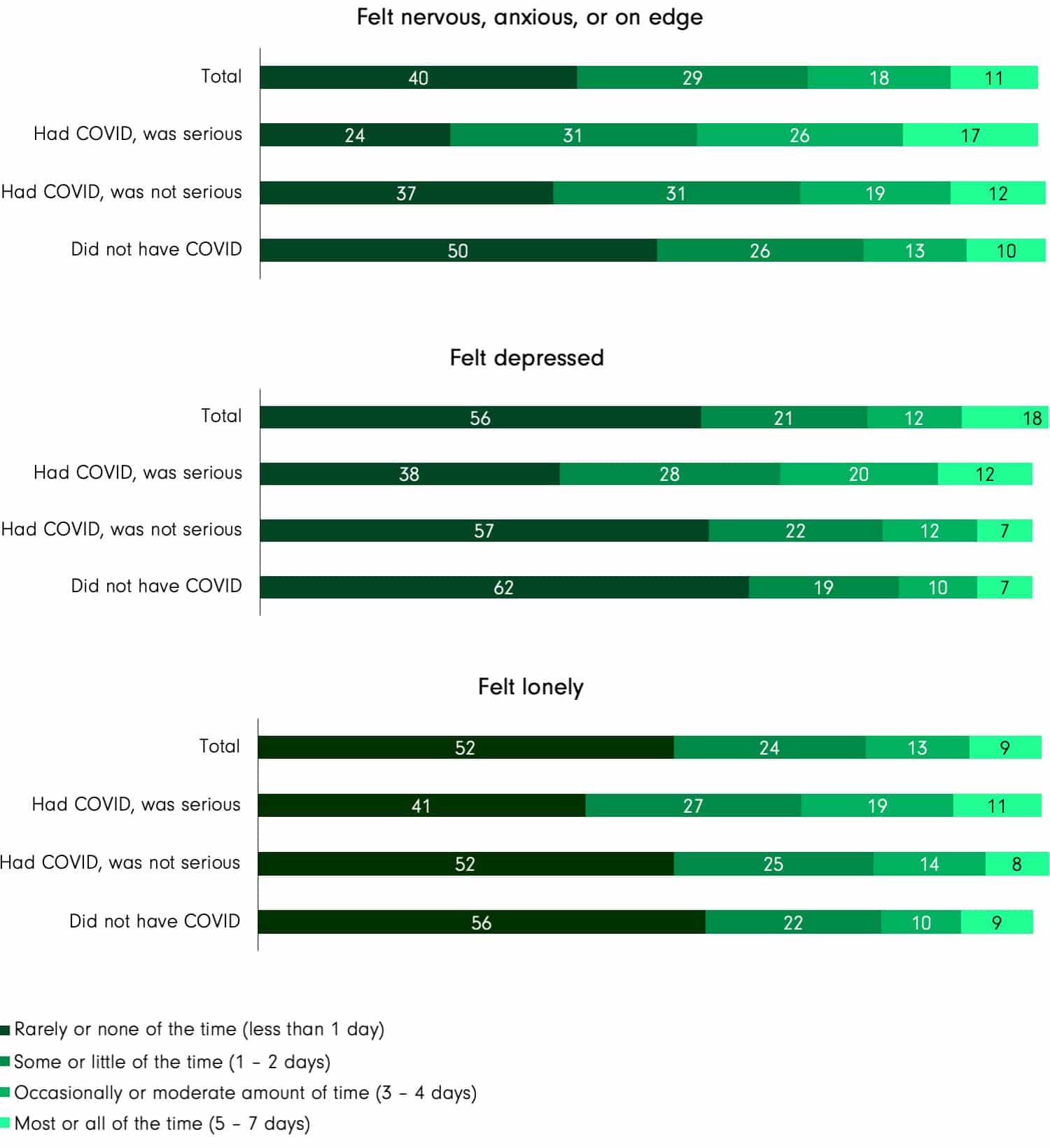
C5. In the past 7 days, how often have you experienced each of the following:
As usual, establishing that there is a relationship between having been seriously ill with COVID-19 and poorer mental health and well-being does not mean that the former necessarily causes the latter – though that remains a possibility. There are, in fact, several different scenarios:
One is that people with poorer mental health were more likely to be seriously affected by COVID-19 (perhaps because their living or economic circumstances placed them at higher risk; or because they were less likely to have access to prompt medical care; or because their mental health was related to other pre-existing physical health conditions that also made them more vulnerable to the coronavirus).
Another is that people who have poorer mental health, or who are more anxious or depressed, assess their physical health situation differently (i.e., more negatively). In other words, they’re more likely to report having had COVID-19 and to describe their illness as serious.
Finally, as mentioned, it could be the case that – for some at least – being seriously ill with COVID-19 (or being ill with COVID-19 for an especially long period of time) has consequences for mental health and well-being that linger even after the physical illness has passed. Among other things, this could be because serious illness can be associated with greater social isolation and heightened economic insecurity.
These scenarios are not mutually exclusive.
Regardless of the explanation, the fact that severe cases of COVID-19 are now more likely to be associated with poorer mental health than with poorer physical health warrants more investigation and discussion. Survey data certainly have limitations in this context: we’re asking people to assess their own health situation in the past and today; their responses can be shaped by many factors that go beyond their actual physical or mental health conditions. But, while it’s fair to treat the findings cautiously, it would be unwise to ignore them. Knowing whether people with poorer mental health are more susceptible to serious illness can help us prepare for and manage future public health emergencies. And knowing whether the mental health impacts of a pandemic linger long after the immediate threat to physical health has past can help us put better supports in place over the longer term.
Finally, these survey results are a reminder that many Canadians are affected by poor health in ways that may remain invisible to their family, friends and co-workers. People who appear physically well or who appear to have recovered from illness may be wrestling with other issues – including anxiety, depression and loneliness – that can’t be detected by a simple test you can pick up at the local pharmacy.
YMCA in Canada 2024 survey
The data in this article are from the YMCA in Canada 2024 survey, conducted by the Environics Institute for Survey Research and YMCA Canada. The survey was conducted online with a representative sample of 2,200 adults Canadians between January 25 and February 2, 2024. The data are weighted by age, gender, region and education to ensure alignment with the actual composition of the Canadian population, based on the 2021 census. The authors would like to thank YMCA Canada for making this data available to them for this analysis, as well as the colleagues who took the time to provide comments on an earlier draft of this article. The authors remain solely responsible for the results and interpretation presented here.
Related reading
A Better Canada: Values and Priorities after COVID-19
Five months after the onset of the COVID-19 pandemic in Canada, the Environics Institute for Survey Research and the Vancouver City Savings credit union joined forces to conduct a comprehensive study of public opinion about what Canadians are expecting from their governments, from corporations and from one another.
September 22, 2020Reportpolitics,COVID-19,social change,democracy
COVID-19 changed everything, except Canada’s values of inclusiveness
While populists around the world have used the pandemic’s many upheavals to sow fears against newcomers, Canada might never have been more sure of its broadly welcoming spirit than now.
January 4, 2021Insightcanadian identity,COVID-19,values,michael adams
The Lingering Effects of COVID-19
This report helps to fill the information gap by documenting how many Canadians have missed work or school due to COVID-19 in the 12 months prior to the time of the survey in March 2023, and the length of their absences.
December 7, 2023Reporteconomy,COVID-19,survey on employment and skills,health


